DISCLAIMER: Patient information provided here does not replace a proper eye examination by a qualified eye care professional. If you are having any problems with your eyes, seek advice from an eye care professional immediately.
Age-Related Macular Degeneration: What is AMD?
AMD is an eye condition and the leading cause of vision loss in North America for those aged 50 and older. It causes damage to the macula leading to loss of your central vision.
AMD can advance so slowly that vision loss does not occur for a long time. In others, the disease can progress faster leading to rapid loss of vision. As AMD progresses, a blurred area near the center of vision is the most common symptom. Over time, the blurred area may grow larger or you may develop blank spots in your central vision. Loss of central vision in AMD can interfere with simple everyday activities, such as the ability to see faces, drive, read, or do close work, such as cooking or writing.
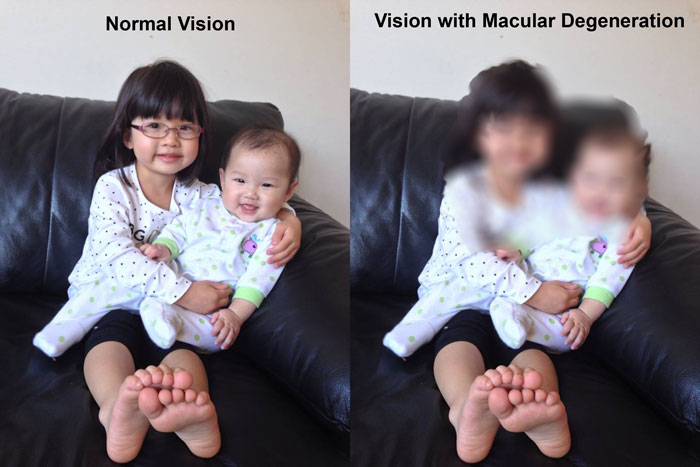
Who is at risk?
Age is the main risk factor for AMD. The disease is most likely to occur after age 50, but it can occur earlier. Other risk factors for AMD include:
- Smoking. Research shows that smoking more than doubles the risk of AMD.
- Race. AMD is more common among Caucasians than among African-Americans or Hispanics/Latinos.
- Family history and Genetics. People with a family history of AMD are at higher risk. Does lifestyle make a difference?
- Poor diet. Research shows that those consuming a poor, unbalanced diet are at a greater risk.
- Life Style: Those that spend more time outdoors unprotected from UV light are at higher risk of AMD.
How is AMD detected?
A comprehensive dilated eye exam can detect help detect even early AMD. The eye exam may include the following:
- Visual acuity test. Testing your vision can determine if there are any deficiencies.
- Dilated eye exam. Optometrists use drops to widen or dilate the pupils. This allows for a better examination of the back of the eye.
- Amsler grid. The Amsler grid is a simple test that can be completed in office or at home to monitor for any potential changes from AMD.
- Optical coherence tomography. You have probably heard of OCT uses high sensitive ultrasound, to image the macula.
How is AMD treated?
The National Eye Institute tested whether taking nutritional supplements could protect against AMD in the Age-Related Eye Disease Studies They found that daily intake of certain high-dose vitamins and minerals can slow progression of the disease in people who have intermediate AMD, and those who have late AMD in one eye. Ask your Optometrist if an eye-related vitamin is suitable for you.
In advanced AMD your Optometrist may refer you to an Ophthalmologist for treatment. Treatment may include injections to stop the progression of the disease.
Glaucoma: What is Glaucoma?
Glaucoma is a family of diseases that damage the eye’s optic nerve and can result in peripheral vision loss and possible blindness. However, with early detection by your Optometrist and with treatment, your eyes can be protected from serious vision loss.

Who is at risk for glaucoma?
Anyone can develop glaucoma, but some additional risk factors are:
- African Americans over age 40
- Everyone over age 60, especially Mexican Americans
- People with a family history of glaucoma
- Anyone with higher pressures in the eye, (not high blood pressure)
Glaucoma Symptoms
At first, with open-angle glaucoma there are no obvious symptoms and it does not cause pain. Vision stays normal. Without treatment or early detection, people with glaucoma will slowly lose their peripheral vision. As glaucoma progresses without treatment the disease can lead to tunnel vision and possible total blindness.
How is glaucoma detected?
Glaucoma is detected through a comprehensive dilated eye exam by your Optometrist that includes the following:
Visual acuity test. The eye chart test measures how well you see at various distances.
Visual field test. This test measures your peripheral (side vision). It helps your eye care professional tell if you have lost peripheral vision, a sign of glaucoma.
Dilated eye exam. Optometrists use drops to widen or dilate the pupils. This allows for a better examination of the back of the eye.
Tonometry is the measurement of pressure inside the eye by using an instrument called a tonometer. Numbing drops may be applied to your eye for this test. A tonometer measures pressure inside the eye to detect glaucoma.
Glaucoma Treatments
Immediate treatment for early-stage, open-angle glaucoma can delay progression of the disease. That’s why early diagnosis is very important.
Glaucoma treatments include medicated eye drops, laser trabeculoplasty, conventional surgery, or a combination of any of these. While these treatments may save remaining vision, they do not improve sight already lost from glaucoma.
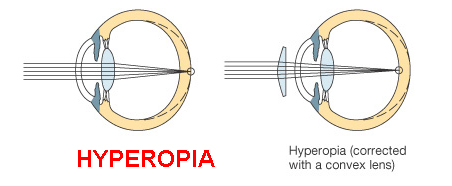
What is hyperopia?
Hyperopia, commonly known as farsightedness, is a type of refractive error where distant objects may be seen more clearly than objects that are near. However, many people experience hyperopia differently. Some people may not notice any problems with their vision, especially when they are young or if the amount of hyperopia is mild. For people with significant hyperopia, vision can be blurry for objects at any distance, near or far. A proper examination with your Optometrist can help determine if you have a refractive error like hyperopia.
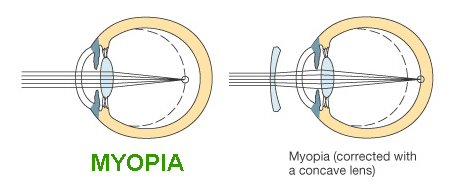
What is myopia?
Myopia, also commonly known as nearsightedness, is a type of refractive error where close objects appear clearly, but distant objects appear blurry. High myopia is a severe form of the condition where the eyeball stretches and becomes too long. This can lead to a high glasses prescription and lead to possible holes or tears in the retina. People with high myopia need comprehensive dilated eye exams more often. Early detection through routine eye examinations can help prevent vision loss.
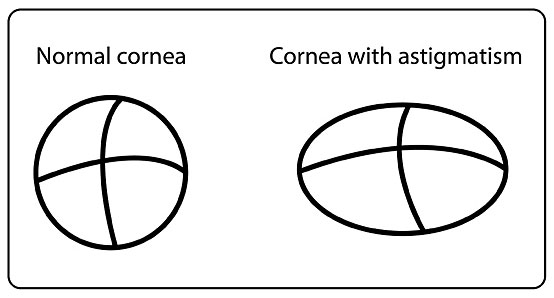
What is astigmatism?
Astigmatism is commonly mistaken as a disease – it is not. Astigmatism is when light is bent differently depending on where it strikes the cornea and passes through the eyeball. The cornea of a normal eye is curved like a basketball, with the same degree of roundness in all around. An eye with astigmatism has a cornea that is curved more like a football, with some areas that are steeper on one side and more rounded on the other side. This can cause images to appear blurry and stretched out. Through your comprehensive eye examination, your Optometrist will be able to determine if you have any astigmatism.
What is a cataract?
A cataract is when the lens inside the eye becomes cloudy. Cataracts are mostly related to aging.. By age 80, more than half of all North Americans either have a cataract or have had cataract surgery.

Who is at risk for cataract?
The risk of cataract increases with age. Other risk factors for cataract include:
- Certain diseases such as diabetes.
- Lifestyle choices such as smoking, alcohol use, and poor diet.
- Prolonged exposure to sunlight or other UV light sources.
- Certain medications increase the development of cataracts.
What are the symptoms of a cataract?
The most common symptoms of a cataract are:
- Cloudy or blurry vision.
- Colors seem faded.
- Glare from lights. A halo may appear around lights.
- Poor night vision.
- Prescription changes in your eyeglasses or contact lenses.
How is a cataract detected?
Cataract is detected through a comprehensive eye exam by your Optometrist that includes:
1. Visual acuity test. Testing your vision can determine if there are any deficiencies.
2. Dilated eye exam. Optometrists use drops to widen or dilate the pupils. This allows for a better examination of the back of the lens in the eye.
3. Brightness Acuity Test. A simple test that helps determine the degree of debilitation from glare.
How is a cataract treated?
A cataract can be removed and replaced with an implantable lens when it is considered mature and/or when the vision loss interferes with everyday activities, such as driving, reading, or watching TV. Your Optometrist will help you determine the optimal time for cataract surgery. Our office can also discuss the advancements and latest technology being offered for cataract surgery.
What can I do to protect my vision and slow the progression of cataract?
Wearing sunglasses and a brimmed hat to block ultraviolet sunlight can help to delay cataract. If you smoke, stop. Researchers also shows good nutrition can help reduce the risk of age-related cataract. We recommend eating green leafy vegetables, fruit, and other foods high with antioxidants.
If you are over 60 years old, you should have a comprehensive dilated eye exam at least once a year. In addition to cataract, your eye care professional can check for signs of age-related macular degeneration, glaucoma, and other vision disorders. Early treatment for many eye diseases may save your vision.
What are floaters?
Floaters appear like little cobwebs or specks that float in your field of vision. They can look like small, dark, shadowy shapes, thread-like strands, or squiggly lines. They move as your eyes move and seem to dart away when you try to look at them directly. They do not always follow your eye movements, and usually drift when your eyes stop moving.
Most people have floaters and learn to ignore them; they are usually not noticed until they become numerous or more prominent. Floaters can become more noticeable when looking at something bright, such as white wall or a blue sky.
What causes floaters?
Most commonly floaters occur when the vitreous, a gel-like substance that fills the eye and helps it maintain a round shape, slowly shrinks.
As the vitreous shrinks, it becomes disrupted and “stringy”, and the strands can cast tiny shadows on the retina. These are floaters.
In most cases, floaters are part of the natural aging process and simply an annoyance. They can be distracting at first, but eventually tend to “settle” away, becoming less noticeable.
There are other, more serious causes of floaters, including, retinal tears. If you experience floaters, flashing lights or large shadows, call an Optometrist immediately. Examination of the eye with dilation drops will help determine if the floaters are from simple vitreous changes or if it is a more serious retinal detachment that may require immediate surgery.
